CDH International’s featured patient of the week is CDH survivor Phoenix-Rose Bax. Her family had this to share about Phoenix-Rose:
“Our daughter, Phoenix-Rose, was diagnosed with congenital diaphragmatic hernia (CDH) at the 20 week scan. We had never heard of this condition so immediately went home and looked on the internet. What we saw made us very worried about what the future might hold. We were referred to St. Georges Hospital for another scan the very next day. This confirmed that our baby had CDH and we were given the decision as to whether we wanted to continue with the pregnancy. An appointment was made for 2 weeks time for another scan and we decided we would give our baby the chance to live and let her decide to fight or give up. The scan showed the severity of her condition gave her a 70% chance of survival but this would depend on whether her lung had developed on the side of the hernia, something that couldn’t be seen via ultrasound. She also had a heart scan which showed her heart was okay but slightly out of position. We were informed that our baby would need to be ventilated as soon as she was born and also saw the neonatal consultant who explained what the operation would entail and the timescales we could be looking at should everything go to plan. It was expected that this should take place between 2 and 10 days after birth so long as she was stable. We had a tour of the neonatal unit and an induction was booked for 5 days before her due date. The pregnancy went well and we tried to keep positive but nothing prepares you for the ups and downs of the following days and weeks after birth.
The birth was straightforward and she was born at 3:14am on Jan 11th 2011 weighing 8lb 12oz, we got to see her for a few minutes once the neonatal team had got her ventilator in before she was taken to intensive care. Dean visited her after an hour or so and returned with all the details and some photos. Despite her size she looked so fragile. She was on an oscillating ventilator which made her little body vibrate and we were told she would need to come off this and on to a regular ventilator before they could operate. We were just grateful that she was alive and had got this far.
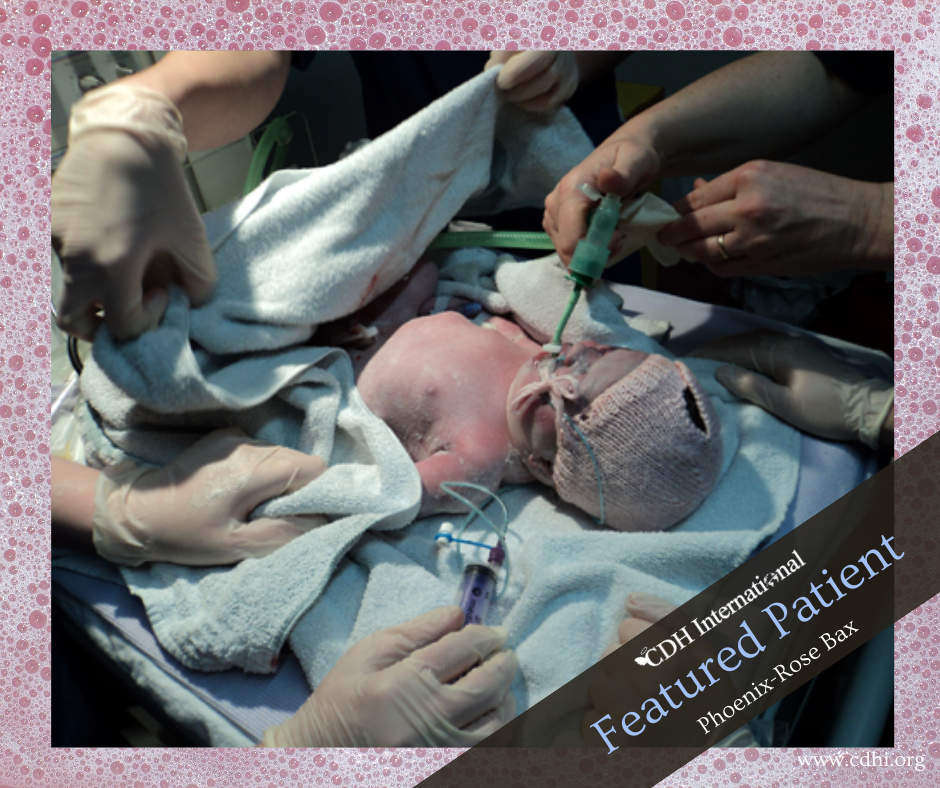
At about day 6 the nurses tried to change her ventilation but she wasn’t happy with it so we had to wait. They tried again at day 8 and this time she seemed ok with it and stable enough by day 9 to be able to have her op. We stayed overnight at the Ronald MacDonald house the night before her operation and sat with her until she was taken to theatre. Trying to keep occupied that day was awful, we went back to the unit at the time she was due back and waited for her, 2 more hours went by and still she hadn’t returned. Of course we thought the worst but she eventually came back, the surgeons said the operation had gone well although it had been more severe than first thought, they delay had been caused by her long line coming out of her cord and having trouble replacing it, this was a continuous problem and was eventually used ultrasound to get a long line in after a few days of trying in a number of different sites. She progressed well, on day 16 her ventilator was removed and she breathed on her own, she was moved to the high dependency room and even had her first tube feed. We were so pleased she was making such good progress and on day 17 got to hold our beautiful baby for the first time.
Day 19 she got an infection and had to be put on a C Pap ventilator and moved back to the intensive care room. After a worrying few days she made slow but steady progress, her feeding was up and down due to suffering quite badly with reflux. She was now having periods off the ventilator and we felt she had turned a corner. The staff at the hospital were great and very supportive, in someways it was quite sad to leave, however almost 1 month after her birth we got the news that she was well enough to move to a hospital closer to home. She arrived at St Peters Hospital were they use a different ventilator and after just 5 days she was off the ventilator, breast and bottle feeding and able to go home. Her 2 older brothers and 2 older sisters who had all visited her in hospital were so pleased to have her home and so were we. She has continued to make good progress, coming off her reflux medication after 4 months. To look at her now you wouldn’t believe the start in life she had. At 10 months old she started to take her first steps.
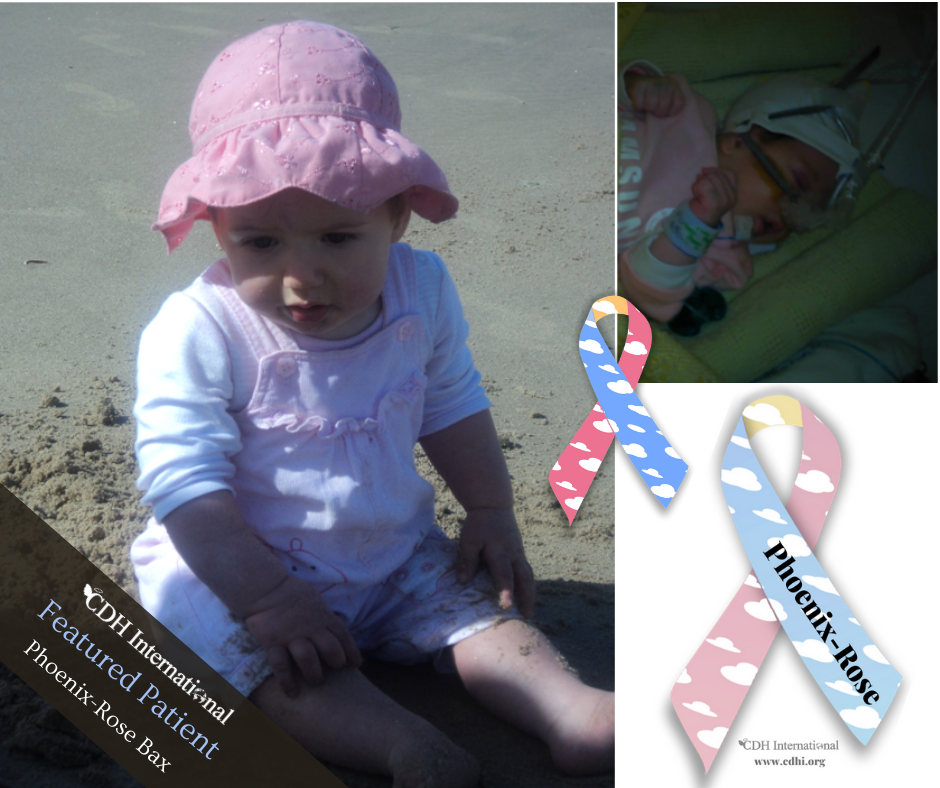
We are so very grateful to all the midwives, nurses, doctors, consultants and surgeons at St Georges who do such a fantastic job. Phoenix-Rose is now 9 years old and doing fantastic.”






